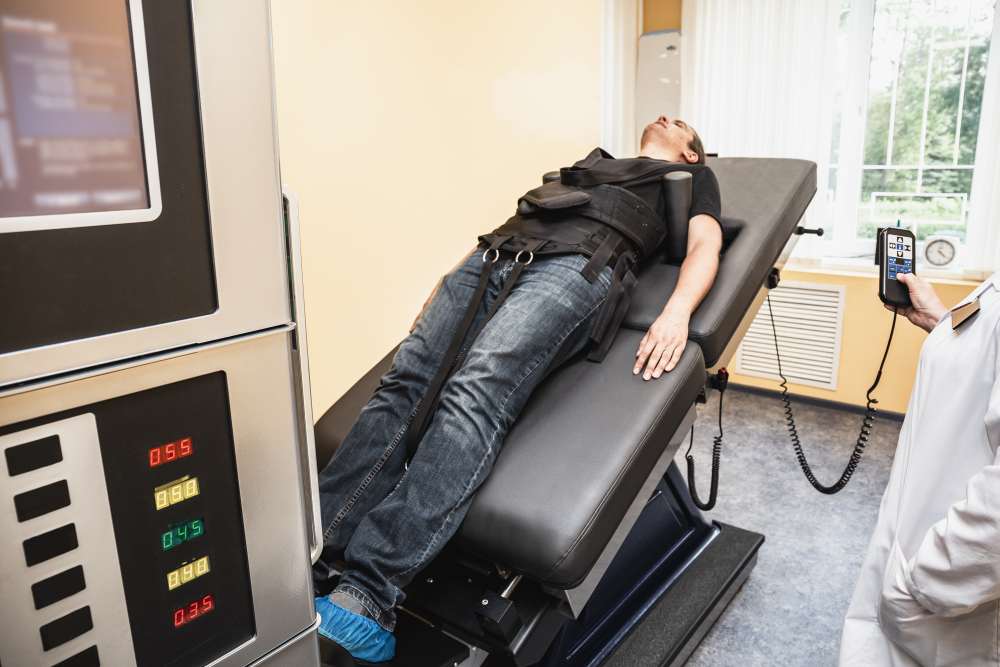
 For the majority of injuries sustained in a car accident, doctors will do their best to use conservative treatment and avoid invasive procedures like surgery. Some emergency situations will require immediate surgery, but other cases may see a patient undergoing surgery much farther down the line. When it comes to back and neck injuries, the best course of treatment is typically focusing on physical therapy and chiropractic care, but that is not always enough. When pain persists or a serious injury occurs, surgery may be necessary. One very common version of this is spinal decompression surgery, especially in the cervical and lumbar spine.
For the majority of injuries sustained in a car accident, doctors will do their best to use conservative treatment and avoid invasive procedures like surgery. Some emergency situations will require immediate surgery, but other cases may see a patient undergoing surgery much farther down the line. When it comes to back and neck injuries, the best course of treatment is typically focusing on physical therapy and chiropractic care, but that is not always enough. When pain persists or a serious injury occurs, surgery may be necessary. One very common version of this is spinal decompression surgery, especially in the cervical and lumbar spine.
Anatomy of the Cervical and Lumbar Spine
While decompression surgery can be performed in all areas of the spine, it is important to understand the difference between each.
The cervical spine refers to the upper region of the spine that supports the neck. Seven vertebrae are a part of the cervical spine, which are labeled as C1 (the top) to C7 (the bottom). Their job is to protect the brain stem and the spinal cord, support the skull, and facilitate a wide range of head motion. Each vertebra has its own anatomy and purpose:
- The first cervical vertebrae (C1) is called the Atlas. It is ring-shaped and primarily supports the skull.
- C2 is known as the Axis. It is circular and has a blunt tooth-like structure, the Odontoid Process or dens, which is projected upward into the Atlas. It helps to enable rotation and turning of the head.
- Vertebrae C3 through C7 are each shaped like boxes, with small projections that extend from the back of the vertebrae.
Beneath the cervical spine is the thoracic spine, which supports the rib cage and ligament systems in the mid-back. The next vertebrae compose the lumbar spine.
The five vertebrae of the lumbar spine are labeled as L1 (the smallest) through L5 (the largest). Each lumbar vertebra is designed to carry the majority of the body’s weight, which is why they are bigger and larger than those throughout the rest of the spine. This region also has more range of motion than the thoracic spine, but not as much as the cervical spine. The lumbar facet joint allows for a lot of flexion and extension movement, but limits rotation.
The next portion of the spine is known as the sacrum, which consists of five bones behind the pelvis.
Common Spinal Injuries After Car Accidents
The spine’s complexity allows for the movements and flexibility that most of us enjoy, but that also means that it is easily damaged. The force of a car accident commonly causes damage to the spine, especially the cervical and lumbar spine. These injuries can range from mild to severe, depending on the accident itself and the spine’s existing integrity.
Whiplash is the most commonly sustained injury after any car accident and is considered a cervical spine injury, though it is a tissue-based injury. In whiplash, the sudden back-and-forth motion of the head causes tissue in the neck to stretch beyond its capacity, leading to strains or even tears. Whiplash that is severe enough can lead to spinal injuries, and the same motion that causes whiplash during impact can also damage the spine. The lumbar spine is subject to some of the same injuries, as well as having its own vulnerabilities.
Some common injuries to the cervical and lumbar spine after a car accident may include the following:
- Cervical spondylolisthesis: One or more vertebrae could slip out of alignment or dislocate due to the force of an accident. This can then compress the spinal cord, causing pain that radiates to the back of the head and shoulders.
- Slipped or herniated discs: The jelly-like discs that sit between vertebrae and absorb shock can be pushed out of place or even rupture due to the force of an accident. This is especially common in the lumbar spine.
- Sprains and strains: Sprains occur when a ligament is torn, while strains damage the facet joint and tendons.
- Pinched nerves: A nerve can become pinched due to damaged tissues, bones, discs, or tendons shifting out of place and compressing or irritating the surrounding nerves. This can lead to severe pain, tingling, or numbness.
- Stiff muscles and tendons: Stiffness in the neck can cause difficulty or pain when moving your head or even keeping your neck in one position for too long.
- Facet joint injury: The facet joint is what allows you to move your head and neck easily and keeps them stable. These joints can be inflamed or irritated during a crash, causing pain.
- Fracture and compression: A fractured cervical spine or broken neck is a very serious injury that requires emergency care. This happens when one or more of the cervical vertebrae is broken or cracked, which can further damage the spinal cord nerves. Without treatment, this can lead to paralysis or death. Fractures in the lumbar spine may be less urgent but are still serious injuries that require treatment.
Most of these injuries can be treated with non-invasive options rather than surgery, with good results. This can include pain-relieving measures like medication, the use of heat and ice, and gentle stretching. Physical therapy and chiropractic care can also be used to manage pain and improve the condition of the spine.
Spinal Decompression Surgery
When more conservative treatment options do not relieve pain and other symptoms, surgery may become an option. Any surgery that removes a structure compressing nerves in the neck is known as cervical decompression surgery. The goal of these surgeries is to leave the spinal structure intact while removing the problematic structures. If this compromises the spine’s integrity, spinal fusion surgery may also need to be performed.
There are multiple types of common spinal decompression surgery, depending on the nature of the injury. These include:
- Foraminotomy: The foramen are openings in the vertebrae where nerve bundles pass through to travel throughout the body. This surgery enlarges this space to relieve pressure on these nerves.
- Laminotomy: The lamina is the bone covering the spinal canal. In this surgery, a hole is created in the lamina to make more space for nerves.
- Laminoplasty: Incisions are made on each side of the lamina to relieve neural pressure, which creates a hinge on one side and a small hole on the other side. A spacer is made of bone, metal, or plastic and inserted into the hole to keep the spinal canal open.
- Corpectomy: When cervical stenosis, a narrowing of the spinal canal, impacts more than one disc, the surgeon can remove the vertebrae along with the discs.
- Microdiscectomy: Also known as microdecompression, this is a minimally invasive procedure that is performed via a small incision in the neck. A small section of the bone is removed over the nerve root, and disc material may be removed as well. This relieves nerve compression and allows the nerve to heal.
- Cervical laminectomy: In the most common surgery for stenosis, the surgeon removes a small section of the lamina to relieve compression on the nerve. The remaining spinal bones are connected back together using titanium metal rods and screws.
Recovering from Spinal Decompression Surgery
 Spinal decompression surgery will usually be performed in a hospital, including about 1 to 4 days of a stay, depending on the complexity of the surgery and your recovery. The majority of people walk unassisted within a day of their operation, though this is gentle movement, and more strenuous activity will be avoided for weeks. It is important to begin moving quickly to avoid developing a blood clot in the leg and to help speed the recovery process.
Spinal decompression surgery will usually be performed in a hospital, including about 1 to 4 days of a stay, depending on the complexity of the surgery and your recovery. The majority of people walk unassisted within a day of their operation, though this is gentle movement, and more strenuous activity will be avoided for weeks. It is important to begin moving quickly to avoid developing a blood clot in the leg and to help speed the recovery process.
Any incisions made during surgery will be closed using stitches or staples, which will need to be removed eventually. You may have a simple dressing placed over the incision that you will need to keep clean and dry until a follow-up appointment.
The recovery process is typically about 4 to 6 weeks. Those who are very physically active in their job may need to take more time off work to heal, however.
It is likely that, during the recovery period, you will engage in physical therapy. The goal of this therapy is to help you regain function and movement in a safe and gentle manner. You should always stick to the routine a physical therapist creates for you to avoid pushing yourself too far and causing more damage.
While complications are rare, spinal decompression surgery does come with risks, like all surgery. These include:
- Infection at the incision site.
- A blood clot developing in a leg vein, known as deep vein thrombosis. In rare cases, this clot can dislodge and travel to the lungs, causing a life-threatening condition known as a pulmonary embolism.
- Damage to the spinal nerves or cords can lead to further pain, numbness and weakness in the legs, or even paralysis.
Your doctor will discuss these risks with you prior to surgery to help determine your eligibility and if you are at additional risk. Surgery, in general, is safer if you do not smoke, generally have good fitness, and are not overweight.
Avoiding Spinal Decompression Surgery
While these surgeries can be very effective, it is generally preferred to avoid such invasive treatment in favor of more conservative remedies. Surgery should only be used when other options are not available or have not produced results or if there is an injury that cannot be treated with other methods.
Avoiding spinal decompression surgery is best done by avoiding conditions that can exacerbate an injury. While all drivers strive to avoid car accidents, this isn’t always possible – however, there are ways to ensure your spine is strong and healthy to avoid as much injury and degeneration as possible. Exercising regularly and maintaining a healthy diet and weight are large factors in your spinal health. People who maintain good physical health in this way may experience less severe injuries after a car accident or be better able to heal if they are injured.
Once an injury has occurred, the best way to avoid it needing surgical treatment is to adhere to a comprehensive care routine created by skilled medical professionals. This exact routine will vary by patient, injury, and a variety of other factors but may include some of the following treatments.
Physical Therapy
After an injury, physical therapy is critical in both relieving pain and regaining function. A physical therapist will help to create a specific exercise routine and other tools that help you to strengthen muscles, improve flexibility and range of motion, and return to a functional level of movement. While pain is often relieved, physical therapy does not always focus on a full eradication of symptoms but on returning to a place where you can live with a high quality of life. Physical therapy is an ongoing treatment and can also be used after surgery to regain abilities.
Chiropractic Care
Some spinal injuries begin with a simple misalignment of the vertebrae, which can be gently corrected via manual chiropractic adjustments. By helping the spine remain aligned, you can prevent the worsening of injury and reduce pain caused by any misalignments. Chiropractic care works with many injuries, but not those like fractures, so it is important to be fully evaluated before using this method.
Injections
If hands-on techniques like physical therapy and adjustments do not relieve pain, injections of corticosteroids into the back may be considered. These treatments are proven to offer long-term relief from pain in many cases and can be a good alternative to surgery.
Your provider may recommend other treatments as well. At AICA Conyers, our team of specialists will work to ensure that your entire health history is taken into account and you are provided with a comprehensive treatment plan. You will work with orthopedists, chiropractors, neurologists, physical therapists, pain relief specialists, and more to ensure you are getting the most holistic care possible. And if surgery does become necessary, our team includes the right people for that as well. Contact us today to get started on healing your back!
